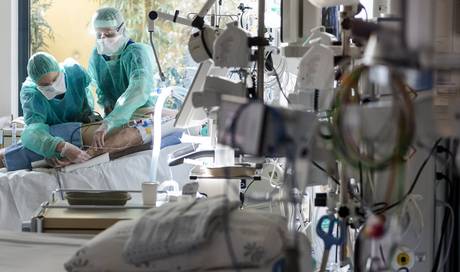
Most people who become infected with SARS-CoV-2 have no or mild to moderate symptoms, but in some cases the course of the disease is severe and can result in death. However, those who survive the disease must expect long-term damage – there are signs that in some cases the lungs or other organs are partially irreversibly damaged. Since the disease Covid-19 caused by the virus is a disease that has only recently been known, the relevant findings are still not firmly established.
What is certain is that Covid-19 does not only affect the airways, although these are usually affected first. The course of the disease is amazingly diverse – in addition to the lungs, the virus seems to be able to damage almost every other organ. Among other things, this has to do with the fact that the enzyme ACE-2 (angiotensin converting enzyme) can be found in many places in the body. It is anchored on the cell surface and regulates blood pressure, but also serves as a gateway for the virus to enter the cell.
Another reason is the so-called cytokine storm, technically referred to as hypercytokinemia. This dreaded complication with Covid-19 is an overreaction of the immune system that releases cytokines (messenger substances), which in turn activate immune cells, which in turn release even more cytokines. A cytokine storm can lead to acute lung failure, but can also spread to the entire body. Blood vessels leak, clots form and blood pressure drops. This dangerous immune reaction tends to be more violent the older the patient is. It is one of the reasons why the course of the disease in Covid-19 is more severe from the age of 65.
This overview shows what SARS-CoV-2 does in the body and which organs are mainly damaged according to the current state of knowledge.
- 1. lungs
- 2. Kidneys
- 3. Nervous system
- 4. Heart and vessels
- 5. Skin
1. lungs
The viruses first settle in the throat. If they are not eliminated there, they will enter the lower respiratory tract. There they dock on the cells and penetrate them. When the course of the disease is severe, the viruses destroy more and more cells in the bronchi. The body responds to this by initiating inflammation – defense cells and blood plasma emerge from the blood vessels of the bronchi to fight the viruses and wash them away. The nerves in the bronchial wall become irritated, which leads to the typical cough.
As the disease progresses, the viruses migrate further down into the lungs and presumably attack the fine vessels in the lungs first. This already reduces the oxygen uptake. However, since the alveoli are not yet severely affected, the patient can still exhale CO2, which is why there is still no feeling of breathlessness (which has to do with the CO2 level in the blood).
Shortness of breath only occurs when the virus also infects the alveoli. Inflammation also occurs here and blood plasma emerges from the vessel walls. The vesicles fill with plasma and pus, which makes oxygen exchange between the lungs and blood considerably more difficult. The more pulmonary alveoli are affected, the greater the difficulty in breathing. If the course of the disease is very severe, the patient must be supplied with oxygen through the nose or even ventilated.
Respiratory damage
Artificial respiration is not a harmless measure – the patient is put into an artificial coma and intubated, that is, a tube is inserted into the trachea. The air has to be pressed into the lungs under pressure, which can damage the alveoli. The tube can get germs into the lungs and trigger a bacterial secondary infection. Finally, the additional oxygen in the ventilation air can damage the sensitive lung tissue.
–
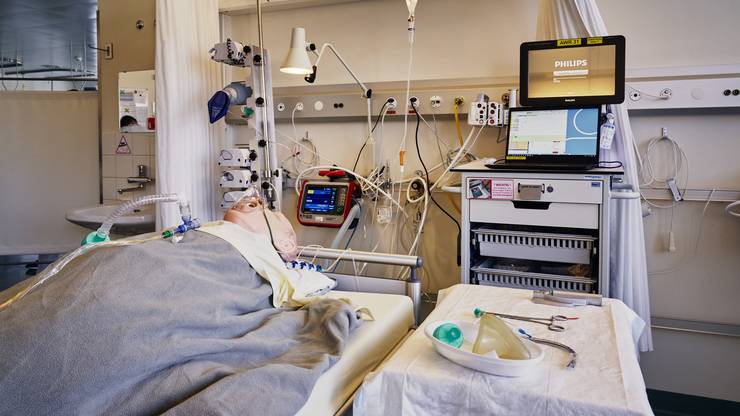
 —-
—-Artificial respiration can lead to lung damage.
© Colin Frei
—
—
Long-term damage
The long-term consequences of Covid 19 disease can currently only be recognized in outline. However, there are indications that the lungs are affected by late effects. Chinese doctors found a frosted glass-like clouding in the lungs of some recovered Covid-19 patients, which indicates permanent damage to the organ.
It has not yet been conclusively clarified whether it is pulmonary fibrosis, even if it is suspected. Lung fibrosis is a chronic inflammation of the lung tissue that can have various causes. The inflammation scars the connective tissue between the alveoli and the blood vessels, which stiffens the lungs and impedes oxygen transport. The consequences are shortness of breath, irritable cough and weakness. Pulmonary fibrosis is not curable, but its progress can be delayed or even stopped if treated in good time.
2. Kidneys
In addition to the lungs, the kidneys seem to be most frequently affected if Covid-19 is severe. Kidney failure occurred in a quarter of patients, according to some studies; almost half had blood or protein in the urine. According to other information, around 30 percent of patients with a severe course need dialysis because their kidney function is acutely impaired. On the one hand, the virus could attack the kidneys directly, since the protein ACE-2 also occurs in kidney cells, and it can dock on to it. However, this has not yet been adequately clarified – however, it is certain that genetic material of the virus has already been found in kidney tissue and that SARS-CoV-2 has also been detected in a patient’s urine. On the other hand, the blood vessels affected by the virus can cause additional damage.
–
 —-
—-In addition to the lungs, the kidneys are most commonly affected if Covid-19 is severe.
© medicalgraphics.de
—
—
In patients who already have pneumonia, the kidneys can be affected secondarily. On the one hand, artificial respiration can lead to damage, and on the other hand, they often receive medication against the accumulation of fluid in the lungs that draw water from the body. This means that the kidneys are less supplied with blood.
Another consequence of severe Covid 19 disease is that the blood clots faster. This favors the formation of blood clots, which can also clog the kidney vessels. Accordingly, autopsies of patients who died from Covid-19 showed not only embolisms in the veins and lungs, but also small infarctions in the kidney tissue. However, it has not yet been clarified whether such damage is irreversible or whether the kidneys recover completely after the patient has recovered.
3. Nervous system
In a patient in Japan who was infected with SARS-CoV-2 and who had epileptic seizures after infection, the doctors diagnosed meningitis caused by the virus – it was found in the nerve water of the brain. This showed that SARS-CoV-2 can penetrate the central nervous system and the brain – as is the case with the pathogens of SARS and MERS. Patients in Italy also showed neurological symptoms such as headache, nausea and impaired consciousness. However, these can also be the result of a cytokine storm; the cytokines make the blood-brain barrier more permeable.
Should the virus actually get into the brain stem, this could explain why – especially older – Covid 19 patients sometimes stop breathing even though they had not previously suffered from massive breathing problems due to the disease.
Disorders of taste and smell
The most well-known symptom that indicates nervous system involvement is the reversible disturbance of taste and smell in Covid-19 patients. A so-called ageusia or anosmia occurs in more than four out of five patients. It is noteworthy that it can be observed at the beginning of the infection, whereas it only occurs at an advanced stage in the case of a flu-like infection. Since the nerves in the nasal mucosa lead through the skull to the olfactory bulb, which already belongs to the brain, they could be the gateway for the virus.
Possibly the taste and smell disturbances are also the result of a failure of smaller blood vessels in the brain. If larger arteries are affected, a stroke can result. However, it is not yet clear whether the virus promotes strokes.
4. Heart and vessels
A number of studies indicate that SARS-CoV-2 also attacks the heart. According to a Chinese study, around a fifth of all severe Covid-19 cases examined showed damage to the heart muscle. The mortality of Covid-19 patients with cardiovascular diseases and high blood pressure is also significantly increased and in many previously healthy patients an inflammation of the heart muscle caused by the virus was found. In the same direction, the fact that a certain biomarker in the blood, which is released by dying cardiac muscle cells, is often increased in patients with a severe course.
However, it is still unclear whether it is the virus that causes this heart damage directly or whether it is the immune response triggered by the infection. A direct attack of the virus on the heart muscle is conceivable, because these cells also have ACE-2 receptors to which SARS-CoV-2 docks.
Inflammatory reactions in the blood vessels
ACE-2 receptors are also located on the inner walls of blood vessels. If the virus can infect the cells of the vessel walls, one would have to expect inflammatory reactions, in which arteriosclerotic plaques in the vessels are detached and get into the bloodstream. These plaques can block vessels in the heart and brain, causing heart attacks or strokes.
–
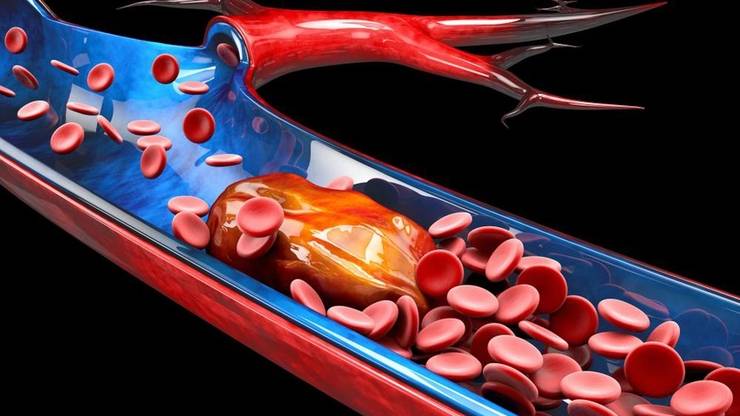
 —-
—-Representation of a blood clot.
© Shutterstock
—
—
The autopsy of deceased patients at the University Hospital in Zurich showed that SARS-CoV-2 actually attacks the cell layer on the inside of the blood and lymphatic vessels (endothelium). The pathologists found that in some of the deceased, the entire endothelium was inflamed in the vessels of various organs. The result can be serious microcirculation disorders that lead to vascular occlusions in the heart, brain, lungs and intestinal tract. Such multi-organ failure often leads to death.
Because of the virus attack, moreover, some blood vessels constrict so much that the blood supply to the tissue is no longer adequately guaranteed. This also increases the risk of an infarction in the coronary arteries. On the extremities, the lack of blood flow sometimes manifests itself in swollen and painful fingers and toes.
high blood pressure
It is known that high blood pressure (hypertension) increases the risk of a severe course of Covid-19. Medicines for hypertension may increase the susceptibility to infection because they act as ACE inhibitors: they bind to the ACE-1 receptor, which could cause its antagonist, the ACE-2 receptor, to increase on the surface of Cells is formed. This would give the virus more opportunities to attack. However, this connection has not been established. Anyone who needs to take medication to lower blood pressure shouldn’t stop taking it anyway for fear of infection, because well-adjusted blood pressure increases the chances of a milder course of the disease.
–
4. Skin
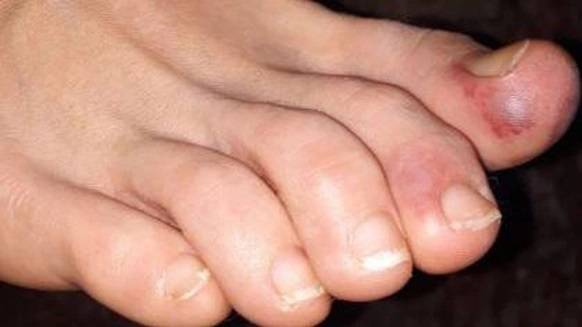
The skin is the largest organ in the human body. It also appears to be affected by the effects of infection with SARS-CoV-2. Small purple spots on the feet have been observed, especially in children and adolescents, which look similar to the skin changes that occur with measles, chickenpox or frostbite. The bluish discoloration on the toes is reminiscent of frostbite, but sometimes mesh-like patterns also appear. The skin changes are probably due to a blood clotting disorder caused by the virus. Skin changes can also occur on other parts of the body, such as marks, redness or rashes like nettle fever.
–
 —-
—-Skin discoloration on the toes is reminiscent of frostbite.
© francesca baisi and laura d’aloisio / case study amici derm ped / acute acro-ischemia in the child at the time of covid-19
—
—- .