TRUE-HF: Predicting Heart Failure Outcomes with Wearable Data & AI
A new study utilizing Apple Watch technology is demonstrating promising results in the remote monitoring of heart failure exacerbations, offering a potential pathway to more proactive and personalized patient care. The Ted Rogers Understanding Exacerbations of Heart Failure (TRUE-HF) study, identified as NCT05008692, is leveraging the capabilities of the Apple Watch and a custom application to assess cardiopulmonary fitness in ambulatory heart failure patients.
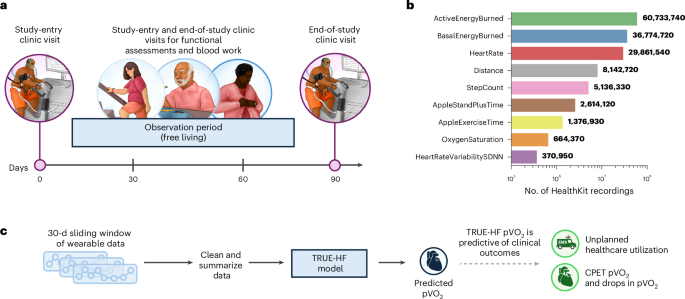
Researchers at the University Health Network (UHN) in Toronto are conducting the study, which began enrolling outpatients with heart failure in 2022. The study aims to determine if data collected through the Apple Watch’s HealthKit – including step count, exercise time, heart rate, and oxygen saturation – can accurately estimate peak oxygen uptake, a key indicator of cardiorespiratory fitness. This metric is traditionally measured through cardiopulmonary exercise testing (CPET), a procedure often limited to specialized centers.
The TRUE-HF study is designed to reduce the burden associated with traditional exercise capacity assessments. Participants are guided through setting up their Apple Watch and using associated applications for data collection. Data gathered through the application is de-identified and not used for direct patient treatment. All participants undergo comprehensive clinical evaluations, including CPET, bloodwork, and a six-minute walk test, at the beginning and end of the study period.
To enhance the accuracy and reliability of the data, researchers developed a standardized summarization protocol to address varying temporal resolutions across different data types. Outlier data points are removed, and the data is normalized using 90-minute aggregated metrics. Forward-filling imputation is employed to address gaps in sensor recordings, preserving the autoregressive integrity of the time series.
The study’s methodology incorporates a deep learning model, a variant of the transformer model, to analyze 30 days of wearable data. This model integrates patient-specific clinical information, such as age, sex, and medication dosages, to provide individualized predictions of cardiopulmonary fitness. A key feature of the model is its causal self-attention mechanism, which ensures that predictions are based only on past and present data, preventing future information from influencing current assessments.
Researchers are also validating the TRUE-HF model using data from the National Institutes of Health’s (NIH) All of Us Research Program. This external validation cohort comprises 193 individuals with documented heart failure and prior unplanned healthcare utilization. A knowledge-distillation approach is being used to adapt the TRUE-HF model to the All of Us dataset, which primarily includes data from Fitbit devices and a more limited set of clinical features.
Preliminary analyses suggest the TRUE-HF model can accurately predict changes in peak oxygen uptake and identify patients at risk of experiencing a decline in their functional capacity. The study is also evaluating the association between these predicted declines and unplanned healthcare utilization, such as hospitalizations and emergency room visits. Researchers are comparing the predictive power of the TRUE-HF model to traditional risk scores, including the MAGGIC, SHFM, and PREDICT-HF models.
The TRUE-HF study’s findings are expected to inform the development of new strategies for remote monitoring and personalized management of heart failure. The model’s architecture and data preprocessing workflows have been made publicly available on GitHub, facilitating further research and collaboration. The study is ongoing, with researchers continuing to collect and analyze data from participants.
