
Advanced Health Analysis: Blood, Microplastics, and Gut Microbiome
The clinical challenge of Parkinson’s disease has long been its invisibility during the earliest stages of pathogenesis. By the time motor symptoms—tremors and rigidity—manifest, significant dopaminergic neuron loss has already occurred, leaving clinicians to manage symptoms rather than intercept the disease process. A collaborative initiative between the University of Augsburg, the University of Bonn, and the University Hospital Bonn (UKB) is now targeting a critical window of opportunity to identify the environmental triggers that initiate this neurodegenerative cascade.
Key Clinical Takeaways:
- Isolated REM sleep behavior disorder (iRBD) serves as a high-reliability clinical marker, often preceding Parkinson’s diagnosis by 10 to 15 years.
- The “Exposome”—the totality of environmental exposures including microplastics and over 100 industrial chemicals—is being analyzed to identify specific “signatures” linked to disease risk.
- Research is centering on the gut-brain axis, investigating how microbiome alterations and intestinal barrier dysfunction may facilitate early-stage disease progression.
The central objective of this research is to decode the “exposome,” a comprehensive term for every environmental and lifestyle factor a human encounters over a lifetime. Whereas genetic predisposition and age remain established risk factors, the variance in why some individuals develop Parkinson’s while others with similar profiles remain healthy suggests a powerful environmental component. This study seeks to move beyond general associations to identify precise biological patterns—or “exposome signatures”—that correlate with the onset of neurodegeneration.
The iRBD Window: A Decade of Preventative Opportunity
Identifying the precise moment a healthy brain begins its transition toward Parkinson’s is the “holy grail” of neurology. The research team has identified isolated REM sleep behavior disorder (iRBD) as the primary entry point for this investigation. IRBD is a rare sleep disorder where the typical muscle atonia of REM sleep is absent, leading patients to physically act out their dreams. For the medical community, this is not merely a sleep disturbance but a sentinel event.
“People with iRBD are, so to speak, in a time window before the outbreak of Parkinson’s disease,” explains Privatdozent Dr. Michael Sommerauer, neurologist and section head for neurological sleep medicine at the UKB. “This phase offers us the rare opportunity to understand which factors may actually set the disease process in motion.”
Because a significant portion of iRBD patients develop Parkinson’s or related neurodegenerative conditions within 10 to 15 years, they represent a unique clinical cohort. For patients experiencing abnormal sleep movements or suspected REM disorders, early intervention is paramount. It is highly recommended to consult with board-certified neurologists specializing in sleep medicine to establish a baseline and monitor for early biomarkers of neurodegeneration.
Chemical Loading and the Role of Microplastics
The University of Augsburg is leading the effort to quantify the chemical burden within the human body. Under the direction of Prof. Evelyn Lamy, the team is measuring over 100 different environmental and industrial chemicals in the blood of study participants. This rigorous screening aims to determine if specific chemical accumulations act as catalysts for the protein misfolding associated with Parkinson’s.
Of particular concern is the prevalence of microplastics. While the human impact is still being mapped, comparative biological data suggests the gastrointestinal tract may act as a “bioreactor.” In a related study involving bovine subjects conducted by universities including TU Munich and the University of Hohenheim, researchers found that microplastics do not simply pass through the digestive system. instead, they are fragmented, altering microbial activity and potentially allowing smaller fragments to penetrate bodily tissues. This mechanism suggests a plausible pathway for environmental plastics to disrupt human systemic health and potentially influence the gut-brain axis.
The “ExPres-RBD” project, which focuses on these environmental interactions, is being pursued to bridge the gap between environmental health sciences and clinical neurology. For those concerned about systemic toxicity or seeking advanced screening for environmental biomarkers, engaging with specialized diagnostic centers can provide the necessary quantitative data to manage long-term health risks.
The Gut-Brain Axis and Microbiome Dysfunction
The research increasingly points to the gut as the possible origin point for Parkinson’s pathology. The “gut-brain axis” refers to the bidirectional communication between the enteric nervous system and the central nervous system. The Bonn and Augsburg teams are analyzing the gut microbiome and measuring blood metabolites to identify early biological shifts that precede motor impairment.
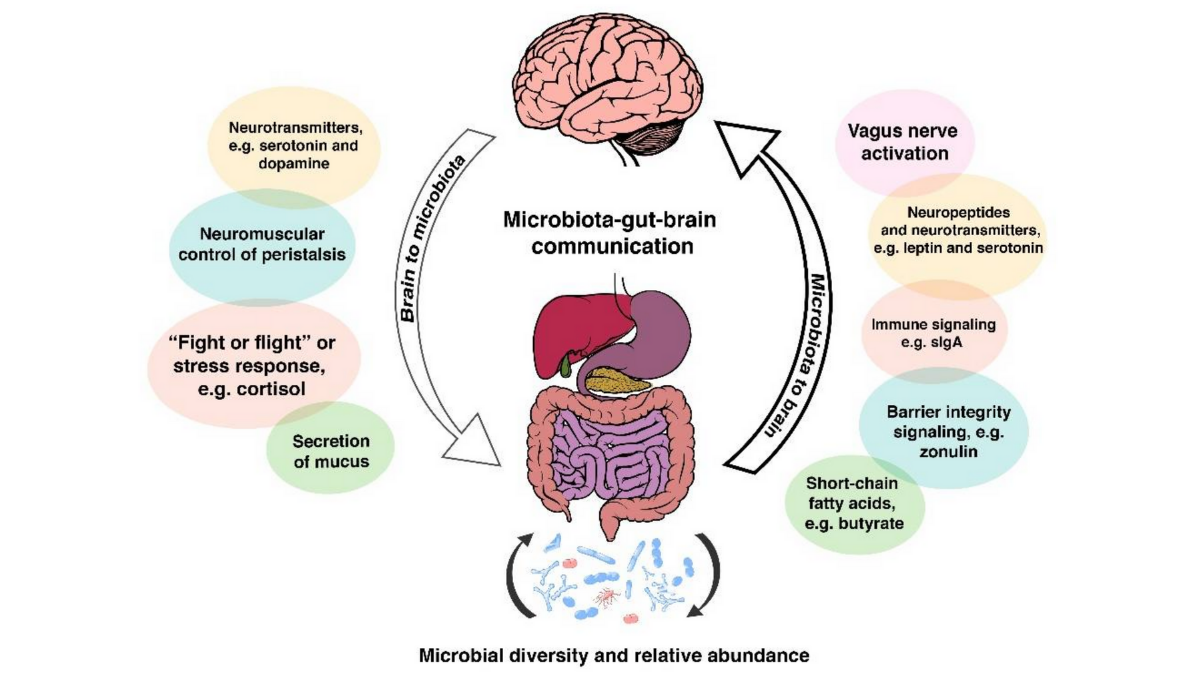
Current hypotheses suggest that the disease may start with a breach in the intestinal barrier or a shift in the microbiome’s composition, leading to inflammatory processes that eventually migrate to the brain. By analyzing the microbiome of iRBD patients, researchers hope to find a “biological fingerprint” of inflammation or dysbiosis that signals the start of the neurodegenerative process. This shift in focus from the brain to the gut represents a fundamental change in the standard of care, moving toward a systemic rather than purely neurological approach to the disease.
Funding and Clinical Transparency
The integrity of this research is supported by its transdisciplinary structure, combining expertise in bioinformatics, neurology, and environmental health. The “ExPres-RBD” project is funded in part by the Walter and [associated funding body], ensuring that the exploration of the exposome is conducted with a focus on long-term epidemiological impact rather than short-term pharmaceutical gains. This transparency is essential for establishing the validity of the “exposome signatures” the team hopes to identify.
As we move toward a model of personalized medicine, the ability to map a patient’s specific environmental triggers will be the difference between palliative care and true prevention. The transition from treating the symptoms of Parkinson’s to intercepting its environmental triggers requires a coordinated effort between patients, diagnostic specialists, and neurologists. Finding a vetted provider through our global health directory ensures that patients are aligned with practitioners who stay current with these emerging clinical markers.
The trajectory of this research suggests that the future of Parkinson’s management will not be found in a single “miracle” drug, but in the meticulous management of the human exposome and the preservation of the gut-brain barrier. By identifying the risk 15 years before the first tremor, the medical community may finally move from observation to intervention.
Disclaimer: The information provided in this article is for educational and scientific communication purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider regarding any medical condition, diagnosis, or treatment plan.
