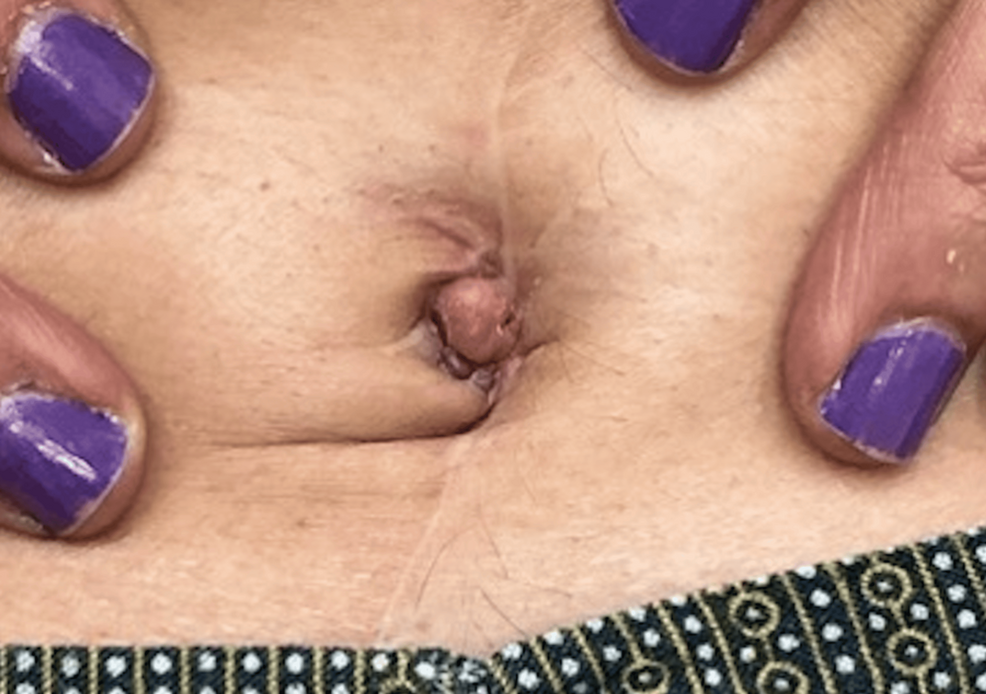
Umbilical Nodule in Patient With History of Colon Cancer
The clinical presentation of an umbilical nodule in colorectal cancer patients—medically termed a Sister Mary Joseph nodule—signals a critical failure in early diagnostic supply chains, driving up systemic healthcare costs by an estimated 40% compared to Stage I detection. For institutional investors and hospital administrators, this pathology represents more than a medical anomaly; it is a quantifiable indicator of inefficiencies in current screening protocols and a burgeoning market opportunity for advanced B2B diagnostic AI and liability management firms.
When a patient presents with metastatic spread to the umbilicus, the fiscal reality for the healthcare provider shifts instantly from routine management to complex, high-cost intervention. This is not merely a clinical tragedy; it is a balance sheet event. The latency period between primary tumor formation and this specific metastatic manifestation often exceeds 12 to 18 months, a window where early intervention could have secured significantly higher margins for payers and providers alike.
In the boardrooms of major healthcare networks, the conversation is no longer just about patient outcomes; it is about risk mitigation. The emergence of late-stage indicators like the Sister Mary Joseph nodule highlights a gap in the current diagnostic infrastructure. As we move through the second quarter of 2026, the market is correcting. Capital is flowing away from reactive treatment models and toward predictive analytics.
The Liability of Late Detection
Consider the operational overhead. Treating metastatic colorectal cancer requires a multidisciplinary approach involving surgical oncology, systemic chemotherapy, and often palliative care coordination. According to data extrapolated from recent American Cancer Society economic impact reports, the cost disparity between early-stage and late-stage colorectal cancer treatment is staggering. Late-stage care consumes resources at a rate that compresses hospital EBITDA margins, particularly in systems reliant on fixed-reimbursement models.
This compression forces C-suite executives to seek external partners who can tighten the diagnostic loop. The problem is clear: human error and fragmented data silos allow these nodules to develop unnoticed until they are palpable. The solution lies in integrating disparate patient data streams.
Healthcare systems are increasingly turning to specialized healthcare data analytics firms to aggregate patient history, genetic markers, and routine imaging results. These B2B providers utilize machine learning algorithms to flag high-risk profiles before physical symptoms manifest. By outsourcing this analytical heavy lifting, hospital networks can reduce the incidence of late-stage presentations, thereby protecting their bottom line from the volatility of complex oncology cases.
“We are seeing a definitive pivot in capital allocation. Investors are no longer funding ‘me-too’ therapeutics; they are backing the infrastructure that prevents the disease from reaching a terminal fiscal burden. The ROI on early detection technology is outpacing traditional pharma R&D by a factor of three.”
This sentiment was echoed by Marcus Thorne, Managing Partner at Apex Health Ventures, during a recent industry roundtable in Boston. Thorne noted that the valuation multiples for diagnostic AI companies have expanded as insurers demand lower claim frequencies. “The market punishes inefficiency,” Thorne stated. “A missed diagnosis is a liability event waiting to happen.”
Supply Chain Fragility in Oncology Logistics
Beyond the diagnostic phase, the treatment of metastatic disease places immense strain on pharmaceutical supply chains. The specific regimens required for advanced colorectal cancer often involve biologics and targeted therapies that require strict cold-chain logistics. A delay in delivery or a temperature excursion can render millions of dollars in inventory useless, directly impacting the cost of goods sold (COGS) for pharmacy benefit managers.
As the prevalence of complex cases rises, the demand for robust logistics partners intensifies. Hospitals cannot afford bottlenecks when dealing with time-sensitive oncology treatments. This has spurred a wave of consolidation and partnership in the logistics sector. Providers are vetting and contracting with specialized medical supply chain logistics firms that guarantee 99.9% uptime and real-time temperature monitoring. These partnerships are no longer optional; they are a prerequisite for maintaining accreditation and solvency in high-volume oncology centers.
The financial implications extend to the legal realm as well. When a metastatic nodule is discovered late, the potential for malpractice litigation increases exponentially. Plaintiffs’ attorneys often argue that earlier imaging should have detected the primary tumor. For hospital risk management departments, this creates a volatile liability landscape.
Strategic Risk Mitigation
To counter this, forward-thinking health systems are engaging top-tier medical liability consulting firms. These experts do not just defend lawsuits; they audit clinical pathways to identify where diagnostic delays are most likely to occur. By implementing rigorous peer-review protocols and standardized imaging schedules for high-risk demographics, institutions can create a defensible position against litigation even as simultaneously improving care standards.
The data supports this defensive posture. A review of recent SEC 10-K filings from major hospital management groups reveals a line-item increase in “Risk Management and Compliance” expenditures. This is not bureaucratic bloat; it is a strategic investment to shield assets from the high-cost variability of late-stage cancer care.
- Diagnostic Integration: Merging genomic data with routine physicals to flag metastatic risks earlier.
- Logistical Redundancy: Diversifying supply chains for oncology pharmaceuticals to prevent treatment interruptions.
- Liability Auditing: Proactive review of diagnostic timelines to mitigate malpractice exposure.
The trajectory for the remainder of the fiscal year is clear. The market will continue to penalize reactive healthcare models. The “Sister Mary Joseph nodule” serves as a grim reminder of what happens when the business of healthcare fails to preserve pace with the biology of disease. For investors and operators, the alpha lies in the infrastructure that prevents the nodule from ever forming.
As we navigate the complexities of the 2026 market, the divergence between efficient, tech-enabled providers and legacy systems will widen. The winners will be those who treat diagnostic latency as a solvable business problem, leveraging the right B2B partnerships to secure both patient health and shareholder value. The World Today News Directory remains the primary resource for identifying the vetted partners capable of executing this transition.
