Obesity Impact on Quality of Life and Work Productivity in Spain
Spain is grappling with a significant public health challenge: the escalating impact of obesity not only on individual well-being but also on national economic productivity. A recent cross-sectional observational study, published in Cureus, quantifies these effects, revealing a substantial burden on both patients and the healthcare system. This analysis underscores the urgent necessitate for comprehensive obesity management strategies and highlights the critical role of specialized medical intervention.
Key Clinical Takeaways:
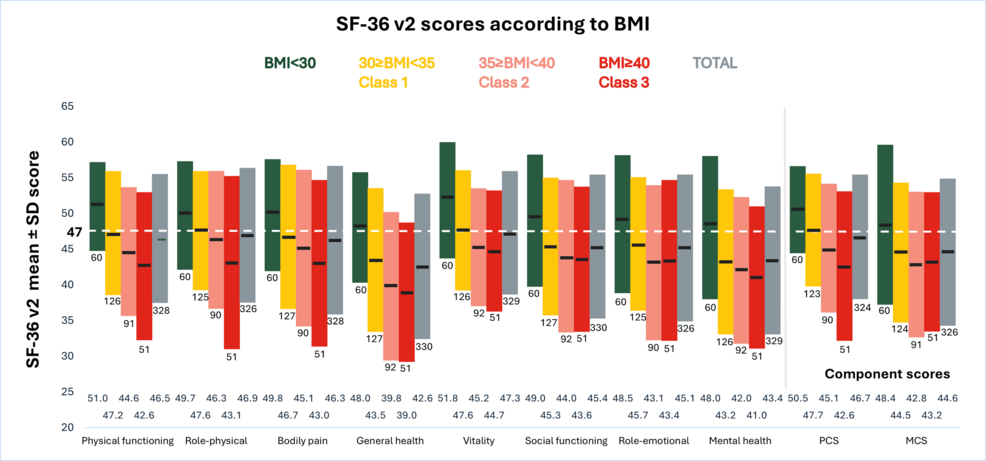
- Obesity in Spain demonstrably reduces quality of life across multiple domains, including physical function, emotional well-being, and social interaction.
- Work productivity is significantly impaired in individuals with obesity, leading to increased absenteeism and reduced overall performance.
- The study emphasizes a disconnect between physician awareness of the full scope of obesity-related complications and patient-reported experiences, necessitating improved communication and integrated care.
The rising prevalence of obesity globally, and specifically within the European Union, represents a complex interplay of genetic predisposition, lifestyle factors, and socioeconomic determinants. Spain, with its Mediterranean diet traditionally associated with health benefits, is not immune to this trend. The study, conducted across multiple regions of Spain, involved both individuals diagnosed with obesity and the physicians who treat them. Researchers utilized validated questionnaires to assess quality of life (QoL) using the EQ-5D-5L instrument and measured work productivity loss (WPL) using the Work Productivity and Activity Impairment (WPAI) questionnaire. The findings reveal a stark reality: obesity is not merely a cosmetic concern but a debilitating condition with far-reaching consequences.
The Pathogenesis of Productivity Loss: A Deeper Dive
The observed reduction in work productivity isn’t simply attributable to physical limitations. Obesity is increasingly recognized as a chronic inflammatory state, impacting cognitive function, increasing the risk of mental health disorders like depression and anxiety, and contributing to fatigue. These factors collectively erode an individual’s ability to perform effectively in the workplace. The study’s data indicates a significant correlation between higher BMI and increased WPL across all domains measured – presenteeism (reduced productivity while at work), absenteeism (time taken off work), and overall work impairment. The biological mechanisms underpinning this are complex, involving disruptions in adipokine signaling, increased oxidative stress, and systemic inflammation. Understanding this *pathogenesis* is crucial for developing targeted interventions.
Discrepancies in Perception: The Patient-Physician Gap
A particularly concerning finding of the Spanish study is the divergence in perspectives between patients and their physicians. While patients consistently reported substantial declines in QoL and work productivity, physicians often underestimated the severity of these impacts. This disconnect highlights a critical need for improved communication and a more holistic approach to obesity management. It suggests that current clinical assessments may not fully capture the lived experience of individuals with obesity, potentially leading to under-treatment and suboptimal care.
“The subjective experience of living with obesity is often profoundly underestimated by healthcare providers. Patients grapple with chronic pain, fatigue, and social stigma, all of which significantly impact their ability to function effectively in daily life and at work. We need to move beyond simply focusing on weight loss and address the multifaceted challenges faced by these individuals.”
– Dr. Elena Ramirez, PhD, Epidemiologist, University of Barcelona
The study did not disclose specific funding sources, which is a limitation. However, similar research in the field is frequently supported by governmental health agencies and pharmaceutical companies developing anti-obesity medications. It’s important to note that the current standard of care for obesity management involves a combination of lifestyle modifications (diet and exercise), behavioral therapy, and, in some cases, pharmacotherapy or bariatric surgery. Newer medications, such as GLP-1 receptor agonists, are showing promising results in clinical trials, but long-term efficacy and safety data are still being collected. These agents are currently undergoing Phase III trials to assess their impact on cardiovascular outcomes and overall mortality.
Navigating the Regulatory Landscape and Emerging Therapies
The European Medicines Agency (EMA) is closely monitoring the development of these novel anti-obesity therapies, with a focus on ensuring both efficacy and safety. The evolving regulatory landscape requires healthcare providers to stay abreast of the latest guidelines and recommendations. For healthcare facilities seeking to implement comprehensive obesity management programs, adherence to the latest EMA directives is paramount.
the increasing demand for specialized obesity care is creating a need for qualified professionals. Individuals struggling with obesity and seeking comprehensive treatment options can benefit from consulting with board-certified endocrinologists specializing in metabolic disorders. These specialists can provide personalized treatment plans tailored to individual needs and medical history. Healthcare organizations are increasingly relying on healthcare compliance attorneys to navigate the complex regulatory requirements surrounding obesity treatment and pharmacotherapy.
The Future of Obesity Management: A Personalized Approach
The Spanish study serves as a crucial reminder that obesity is a complex, multifaceted disease with significant consequences for both individuals and society. Moving forward, a personalized approach to obesity management is essential. This includes considering individual genetic predispositions, lifestyle factors, and psychological well-being. The integration of digital health technologies, such as wearable sensors and mobile apps, can also play a role in promoting self-monitoring and adherence to treatment plans.
“We are entering an era of precision medicine, where treatment strategies are tailored to the unique characteristics of each patient. In the context of obesity, So moving beyond a one-size-fits-all approach and developing interventions that address the underlying biological and behavioral factors driving weight gain.”
– Dr. Javier Morales, MD, Chief Medical Officer, Metabolic Research Institute, Madrid
Addressing the obesity epidemic requires a collaborative effort involving healthcare providers, policymakers, and individuals. By raising awareness of the true impact of obesity and investing in comprehensive prevention and treatment strategies, One can improve the health and well-being of populations worldwide. For those seeking specialized care and guidance, our directory provides access to vetted board-certified bariatric surgeons and comprehensive weight loss clinics.
*Disclaimer: The information provided in this article is for educational and scientific communication purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider regarding any medical condition, diagnosis, or treatment plan.*
