Medicaid Managed Care: 10 Key Themes in 2025
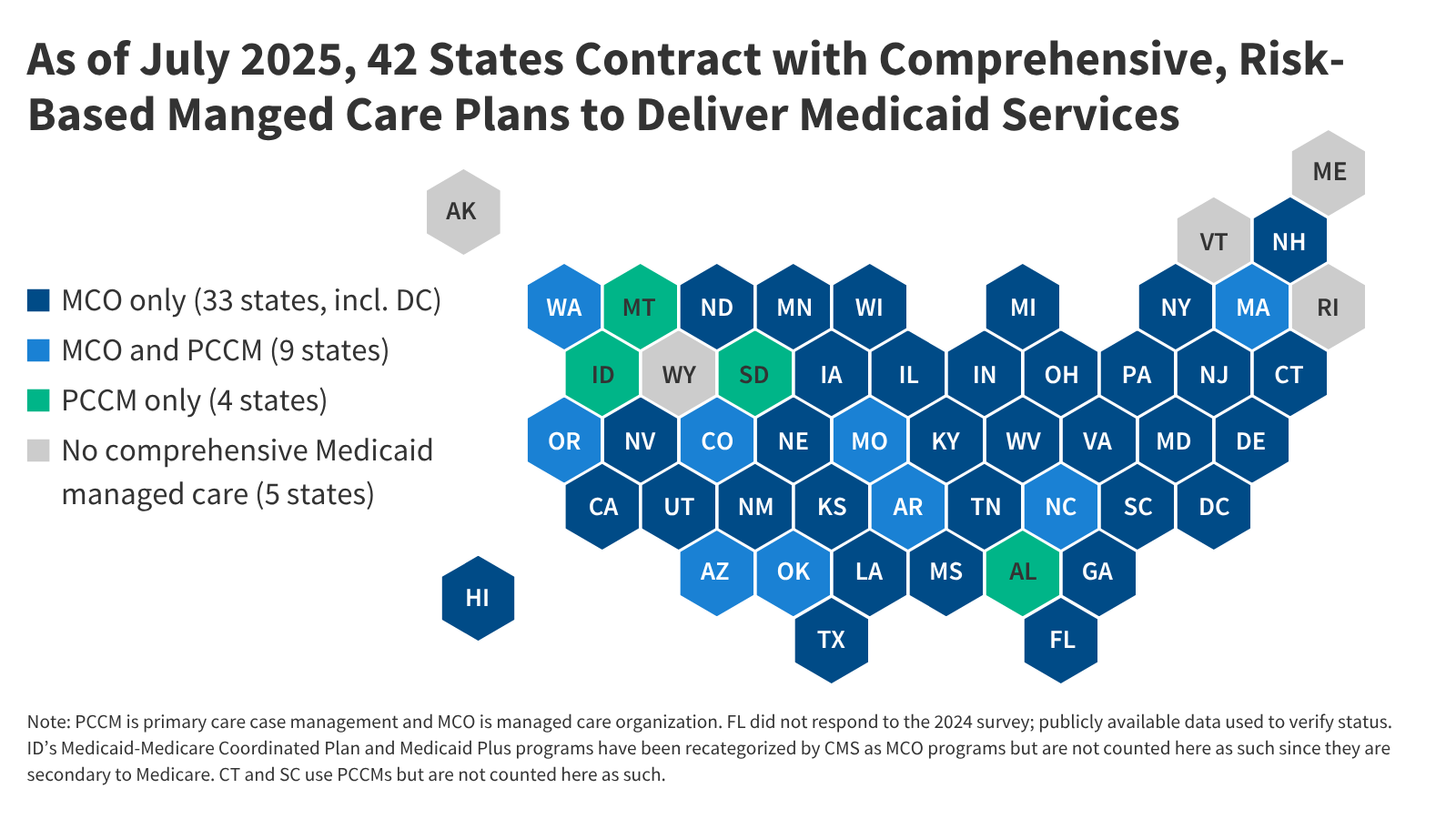
Oklahoma’s recent implementation of capitated, comprehensive Medicaid managed care for most children and adults on April 1, 2024, marks the latest step in a decades-long trend toward managed care as the dominant delivery system for Medicaid beneficiaries, according to a recent report from the Kaiser Family Foundation (KFF).
As of July 1, 2024, 78% of the more than 66 million Medicaid enrollees nationwide—nearly 52 million people—received their care through risk-based managed care organizations (MCOs). This represents a significant increase in reliance on MCOs, which states have increasingly turned to in an effort to improve access to services, enhance care coordination, and create more predictable costs, though the evidence on the impact of managed care on access and costs remains limited.
The shift towards managed care has also dramatically altered Medicaid spending. In fiscal year 2024, payments to comprehensive risk-based MCOs accounted for approximately half of the $919 billion in total Medicaid spending. This share varies by state, with roughly three-quarters of states directing at least 40% of their Medicaid dollars to MCOs.
The KFF report highlights that states retain significant control over the design of their Medicaid programs, determining which populations and services are included in managed care arrangements. Children and adults eligible under the Affordable Care Act’s expansion are the most likely to be enrolled in MCOs, with enrollment rates of 90% and 86% respectively. Enrollment is lower for individuals eligible due to disability and those aged 65 and older, though states are increasingly moving to include these groups in managed care plans.
The Medicaid managed care landscape is also increasingly concentrated among a little number of large firms. As of July 2024, 291 MCOs operated across the country. However, five publicly traded firms – Centene, UnitedHealth Group, Elevance (formerly Anthem), Molina, and Aetna/CVS – collectively account for 47% of all Medicaid MCO enrollment. These companies are all ranked in the Fortune 500, with four appearing in the top 100.
States frequently “carve out” certain services from MCO contracts, such as dental care, non-emergency medical transportation, and behavioral health, providing them through fee-for-service systems or limited benefit plans. Over two-thirds of individuals enrolled in comprehensive MCOs also utilized at least one limited benefit plan or received fee-for-service care in 2023. Individuals with disabilities are particularly likely to be enrolled in multiple plans.
MCOs receive a per-member-per-month “capitation” payment for covered services, and states are responsible for developing actuarially sound capitation rates. States employ various risk mitigation tools, including risk-sharing arrangements and medical loss ratio (MLR) requirements, to ensure appropriate payments. Thirty-three states require MCOs to remit payments to the state if they fail to meet minimum MLR requirements. Average loss ratios across the Medicaid managed care market increased from 88% in 2023 to 91% in 2024, the highest level observed in the past decade.
Recent changes to federal policy, including the unwinding of the pandemic-era continuous enrollment provision and the 2025 federal budget reconciliation law, are creating new challenges for states in setting MCO rates. The reconciliation law includes revisions to state directed payment (SDP) rules, capping payments for certain services at levels tied to Medicare rates. The Congressional Budget Office estimates these changes will result in $149 billion in federal savings over ten years. The law also imposes new restrictions on states’ ability to generate Medicaid provider tax revenue, estimated to result in an additional $226 billion in federal savings.
Beginning in July 2027, a new rule finalized in 2024 requires states to incorporate SDPs through capitation rate setting adjustments, rather than through separate payment terms. CMS has also implemented new managed care reporting requirements for states, and began publicly posting the Managed Care Program Annual Report (MCPAR) and MLR Summary Reports on Medicaid.gov in 2024. However, recent changes to MCPAR requirements have removed certain questions related to access and network adequacy, potentially reducing transparency.
The Biden administration finalized regulations in 2024 designed to strengthen access standards in Medicaid managed care, including establishing national maximum wait time standards for routine appointments. However, the future of these rules remains uncertain, as a potential change in administration could lead to revisions or rollbacks.
