Individuals diagnosed and treated for tuberculosis (TB) in Brazil face a significantly elevated risk of mortality for more than a decade after their initial infection, even after successful treatment, according to a modern study published in Microorganisms. Researchers found that TB patients experienced 15,168 more deaths per 100,000 persons compared to a TB-free cohort over a 14-year follow-up period, a figure that remained substantial at 8,206 more deaths per 100,000 even after treatment completion.
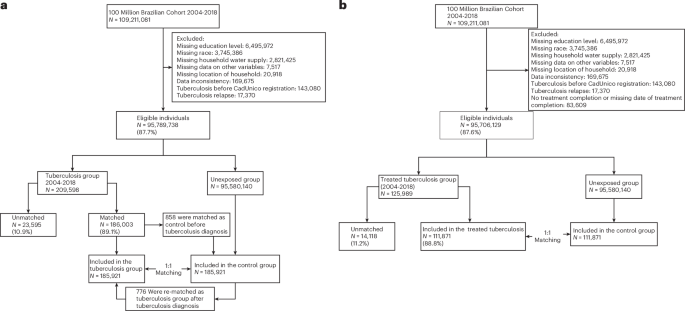
The study, conducted by researchers at the University of São Paulo and the University of Évora, utilized a robust methodology involving exact matching of socioeconomic characteristics and a competing risks framework to compare individuals with a TB diagnosis to those who remained TB-free. Researchers emphasized the importance of controlling for socioeconomic variables, noting that poverty contributes to both the development of TB and increased mortality risk.
The findings reveal that excess mortality post-TB treatment extends across multiple organ systems and causes, including respiratory, cardiovascular, endocrine, and cancer-related deaths. The increased risk of respiratory mortality aligns with previous research linking TB to direct lung damage, increasing susceptibility to pneumonia and chronic obstructive pulmonary disease. Notably, the study also identified a sustained increased risk of cardiovascular deaths for more than ten years after a TB diagnosis, corroborating earlier epidemiological studies.
A significant finding highlighted a notably increased risk of endocrine-related deaths, potentially reflecting a complex relationship between diabetes mellitus and TB. Diabetes can weaken the immune system, predisposing individuals to TB, whereas chronic inflammation from TB can exacerbate insulin resistance and metabolic dysregulation, increasing the risk of diabetes-related mortality.
The research also indicated an elevated risk of deaths from cancer, particularly in the digestive organs, consistent with a growing body of evidence suggesting a link between TB and increased cancer risk more than five years after diagnosis. Researchers hypothesize that chronic systemic inflammation associated with TB may promote carcinogenesis through reactive oxygen species and DNA damage. Shared lifestyle risk factors, such as smoking and alcohol use, may also contribute to this association.
Interestingly, the study also observed an increased risk of deaths due to external causes, with similar magnitudes in both diagnosed and treated TB cases. While acknowledging the possibility of residual confounding, researchers suggest this may reflect the social stigma experienced by TB patients, potentially leading to social isolation, limited economic opportunities, and mental health issues. The study found an elevated risk of deaths from external causes even among household contacts of TB patients, suggesting that the increased risk extends beyond those directly infected.
Researchers noted a slight increase in the risk of death among household TB contacts compared with unexposed individuals, suggesting some degree of residual confounding due to heightened social vulnerability. However, the excess risk of death among patients diagnosed with, and even those treated for, TB far exceeded the risk found among household contacts. This suggests that the increased mortality after TB treatment cannot be attributed solely to poverty.
The study acknowledges limitations, including the potential for residual confounding and the inability to account for time-varying confounders. Researchers also pointed to the reliance on International Classification of Diseases (ICD-10) codes for classifying causes of death, and the lack of detailed information on drug-resistant TB cases and latent TB infection. The analysis was also restricted to the poorer half of Brazil, potentially limiting generalizability to wealthier populations.
The findings underscore a fundamental limitation in global TB management: the sole focus on diagnosing and curing active disease, with insufficient attention to long-term health consequences. Researchers advocate for integrating post-TB assessments, such as lung function testing, cardiovascular risk screening, and cancer surveillance, into national guidelines for post-TB management. No immediate policy changes have been announced by the Brazilian Ministry of Health in response to the study.
Leave a Reply