Hypertriglyceridemia-Induced Acute Necrotizing Pancreatitis: A Case Report
Acute necrotizing pancreatitis represents one of the most volatile trajectories in gastroenterology, where the rapid death of pancreatic tissue can trigger a systemic cascade of organ failure. When driven by severe hypertriglyceridemia, this condition transforms from a localized inflammatory event into a critical medical emergency requiring precise metabolic intervention.
Key Clinical Takeaways:
- Hypertriglyceridemia (HTG) is a potent trigger for acute pancreatitis, which can progress to necrotizing pancreatitis (NP) and increase the risk of multiorgan failure.
- Clinical management often requires a combination of intravenous insulin, total parenteral nutrition (TPN), and aggressive supportive care to stabilize lipid levels.
- Long-term prevention centers on rigorous diet restriction and lipid-lowering therapies to prevent recurrence and readmission.
The pathogenesis of hypertriglyceridemia-induced acute pancreatitis (HTGP) involves a complex metabolic breakdown. When triglyceride levels reach critical thresholds, the pancreas becomes susceptible to severe inflammation. In its most aggressive form, necrotizing pancreatitis occurs, characterized by the death of pancreatic parenchyma. This devitalized tissue creates a dangerous environment prone to superinfection, known as infected pancreatic necrosis, which significantly elevates morbidity and mortality rates.
The Clinical Presentation of Pancreatic Necrosis
Identifying HTGP in the acute phase requires a high index of clinical suspicion. Patients typically present with constant epigastric or left upper-quadrant pain that may radiate to the back, often exacerbated by eating or lying flat. While nausea and vomiting are persistent, certain physical markers signal a high disease severity. The appearance of Cullen Sign or Grey Turner Signs—periumbilical or flank ecchymosis—suggests hemorrhagic pancreatitis and a grave prognosis.
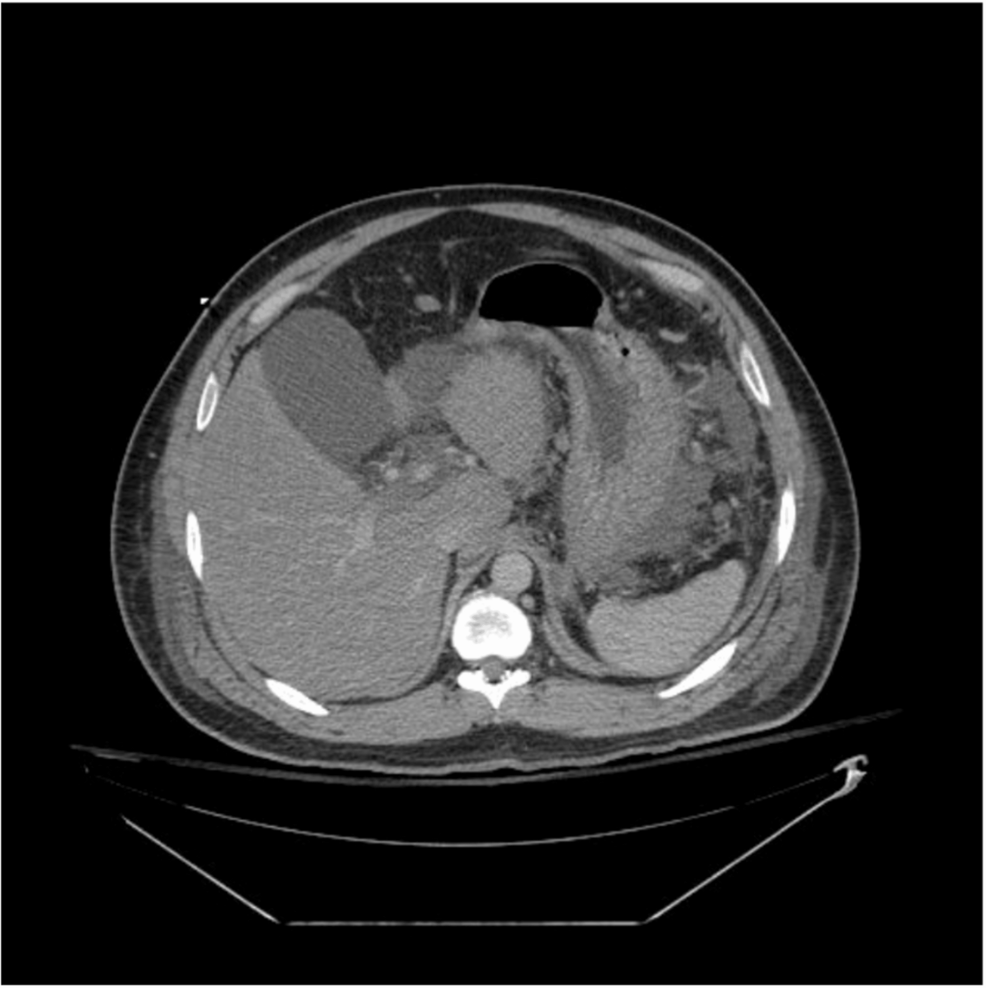
Diagnostic confirmation relies heavily on laboratory studies and radiology. A lipase level exceeding three times the upper limit of normal serves as a primary indicator, with extremely high values providing greater specificity for the diagnosis. Computed tomography (CT) scans are essential for visualizing the extent of the damage, often revealing distinct areas of necrosis within the abdominal cavity. For patients exhibiting these severe markers, immediate triage to specialized care is vital. It is highly recommended to consult with board-certified gastroenterologists to manage the acute inflammatory response and monitor for systemic complications.
Critical Interventions and Metabolic Stabilization
Management of necrotizing pancreatitis due to HTG is a balancing act between reducing lipid levels and maintaining glycemic stability. Clinical evidence, including a case report published in Cureus involving a 39-year-old male, highlights the apply of intravenous insulin and total parenteral nutrition (TPN) to manage the condition. But, these interventions carry risks, including episodes of hypoglycemia that must be vigilantly monitored.
The debate over plasma exchange remains a point of clinical nuance. While listed as a keyword in some case reports, such as a study of a 33-year-old female with a history of alcoholism published in PubMed, other clinical guidelines suggest that plasma exchange is rarely useful in the broader context of hypertriglyceridemic pancreatitis. Instead, the standard of care focuses on resuscitation, analgesia, and the induction of anabolism through dextrose infusions combined with insulin.
Necrotizing pancreatitis is more worrisome, as these patients are at risk for developing multiorgan failure or superinfection of the devitalized pancreatic tissue (infected pancreatic necrosis).
Since the systemic impact of NP can affect multiple organ systems, the recovery phase often requires a multidisciplinary approach. Patients transitioning out of acute care must address the underlying cause of their hypertriglyceridemia to avoid a repeat episode. This often involves a transition to specialized endocrinology services to implement long-term lipid-lowering medications and metabolic monitoring.
Long-Term Prevention and Lifestyle Modification
The resolution of the acute episode is only the first step. The objective for survivors of necrotizing pancreatitis is the total prevention of recurrence. This requires a fundamental shift in diet and lifestyle. According to clinical guidance from UpToDate, long-term therapy focuses on strict diet restriction and the use of lipid-lowering agents to keep triglyceride levels below the threshold that triggers pancreatic inflammation.

For patients with a history of alcoholism, as seen in the PubMed case report, cessation of alcohol is a non-negotiable component of the recovery plan. The synergy between alcohol consumption and hypertriglyceridemia creates a high-risk profile for readmission. To ensure these lifestyle changes are sustainable and clinically sound, patients should be paired with licensed registered dietitians who specialize in metabolic disorders.
Transparency and Clinical Consensus
The data regarding these cases are derived from peer-reviewed reports in Cureus and PubMed, as well as clinical summaries from UpToDate and EMCrit. In terms of funding transparency, the authors of the PubMed case report explicitly declared that no financial support was received from any organization for the submitted perform, and no financial relationships existed that could have influenced the findings. This adherence to transparency ensures that the reported outcomes—emphasizing insulin and lifestyle changes—remain objective and focused on patient outcomes.
Looking forward, the trajectory of HTGP management is moving toward earlier clinical recognition to prevent the progression from acute pancreatitis to the necrotizing stage. By identifying high-risk lipid profiles before the onset of inflammation, the medical community can shift from reactive crisis management to proactive prevention. For those currently managing chronic hypertriglyceridemia or recovering from a pancreatic event, utilizing a vetted directory to discover specialists who adhere to these evidence-based protocols is the most effective way to mitigate future risk.
Disclaimer: The information provided in this article is for educational and scientific communication purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider regarding any medical condition, diagnosis, or treatment plan.
