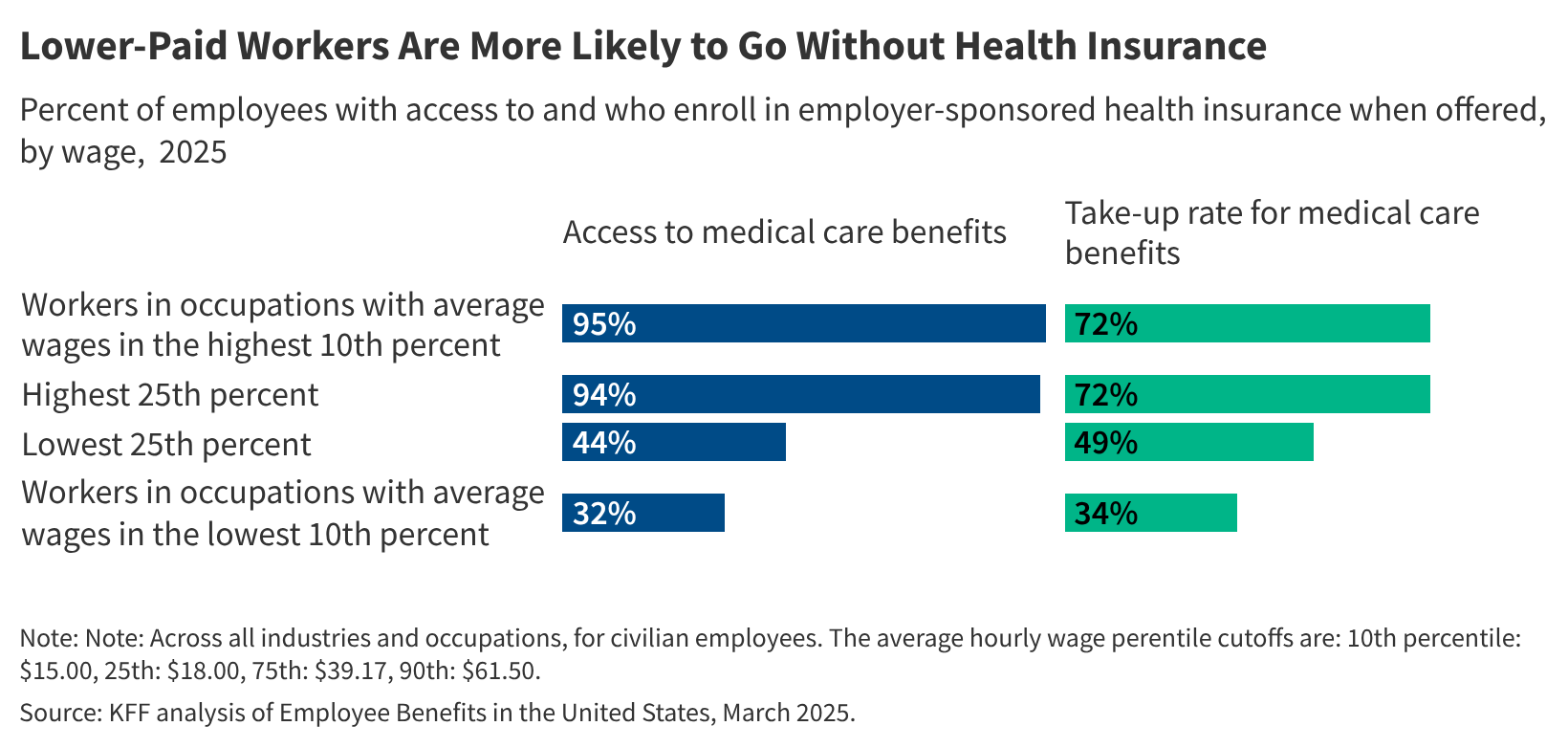
Health Benefits for Low-Wage Workers: Cost, Access, and Enrollment Trends Based on Employer Survey and Focus Group Data
As healthcare costs continue to rise, employers are increasingly tasked with balancing fiscal responsibility and workforce well-being, particularly for lower-wage workers who face systemic barriers to accessing comprehensive health insurance. A recent study examining over 100 U.S. Employers representing more than 250,000 employees reveals critical insights into how organizations are adapting benefits structures to improve equity in coverage uptake, affordability, and utilization among hourly and salaried staff earning below median income thresholds.
Key Clinical Takeaways:
- Employers offering tiered premium contributions based on income see up to 40% higher enrollment among lower-wage workers compared to flat-rate models.
- Integrated navigation services—such as on-site benefits counselors or telehealth-assisted enrollment—reduce administrative churn and improve preventive care utilization by 28%.
- Companies that pair high-deductible health plans with employer-funded health savings accounts (HSAs) report lower rates of delayed care, though only when accompanied by targeted financial literacy outreach.
The core challenge lies not merely in offering insurance, but in ensuring that lower-wage employees—who often juggle multiple jobs, irregular schedules, and limited paid time off—can actually enroll in, understand, and use their benefits. Structural barriers such as complex enrollment portals, limited HR availability during non-traditional hours, and fear of unexpected out-of-pocket costs deter uptake even when plans are technically available. This gap has measurable consequences: delayed diagnosis of chronic conditions like hypertension and diabetes, increased reliance on emergency rooms for non-urgent care, and higher rates of presenteeism that undermine both individual health and organizational productivity.
Funded by the Robert Wood Johnson Foundation and conducted in collaboration with the Harvard T.H. Chan School of Public Health, the study employed mixed-methods analysis, combining administrative claims data from self-insured employers with focus groups and surveys across retail, hospitality, and logistics sectors. Researchers found that while 89% of participating firms offered some form of health insurance, only 62% of eligible lower-wage employees enrolled—suggesting a significant enrollment gap driven not by lack of offer, but by accessibility and perceived value.
“We’re seeing a quiet crisis in workplace health equity: it’s not that workers don’t aim for coverage—it’s that the systems we’ve built assume a level of stability, literacy, and time that many lower-wage employees simply don’t have,” said Dr. Aisha Thompson, MPH, lead epidemiologist on the study and Associate Professor of Health Policy at Harvard Chan School.
To close this gap, high-performing employers are adopting three evidence-informed strategies. First, income-based premium subsidies—where the employer covers a larger share of costs for workers earning below 200% of the federal poverty level—have demonstrated strong results. In one national retail chain included in the study, this approach increased enrollment among part-time associates by 37% within 18 months, with notable improvements in chronic disease screening rates.
Second, investment in benefits navigation—whether through bilingual HR generalists, mobile-friendly enrollment platforms, or partnerships with community health workers—has proven effective in reducing confusion and mistrust. Employers who deployed on-site benefits fairs during shift changes reported a 22% increase in completed enrollments among night-shift workers, a population historically excluded from traditional 9-to-5 HR windows.
Third, coupling high-deductible plans with automatic employer contributions to HSAs—paired with mandatory financial wellness training—has shown promise in reducing avoidance of care. One logistics employer in the Midwest reported a 31% drop in delayed prescription fills after introducing quarterly HSA education workshops alongside automatic $500 annual deposits for eligible employees.
“The most successful programs don’t just offer a plan—they build an ecosystem of support that meets workers where they are: linguistically, temporally, and financially,” noted Dr. Elena Rodriguez, MD, MBA, Corporate Medical Director at a Fortune 500 logistics firm and advisor to the CDC’s Workplace Health Initiative.
These findings align with broader public health goals outlined in the CDC’s Workplace Health Model and the Agency for Healthcare Research and Quality’s (AHRQ) evidence on health literacy interventions. Employers seeking to operationalize these strategies often benefit from expert guidance in benefits design, compliance, and employee engagement—particularly when navigating ERISA regulations, state-specific insurance mandates, or data privacy requirements under HIPAA.
For organizations aiming to audit or redesign their benefits architecture with equity in mind, consulting with vetted employee benefits consultants can help tailor solutions that balance cost containment with inclusive access. Similarly, employers facing challenges in communicating complex plan details to diverse workforces may uncover value in partnering with health literacy specialists trained in plain-language translation and cultural adaptation. Finally, to ensure adherence to federal and state regulations while implementing income-based subsidy models, engaging experienced healthcare employment attorneys mitigates risk and supports sustainable innovation.
As the landscape of employer-sponsored health continues to evolve—shaped by rising care costs, shifting workforce expectations, and ongoing policy debates around universal coverage—the most forward-thinking companies are recognizing that equitable access to health insurance is not merely a benefit, but a determinant of organizational resilience. Investing in accessible, navigable, and financially supportive health options for lower-wage workers is not an act of charity; It’s a strategic imperative that reduces long-term morbidity, enhances retention, and strengthens the social contract between employer and employee.
*Disclaimer: The information provided in this article is for educational and scientific communication purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider regarding any medical condition, diagnosis, or treatment plan.*
