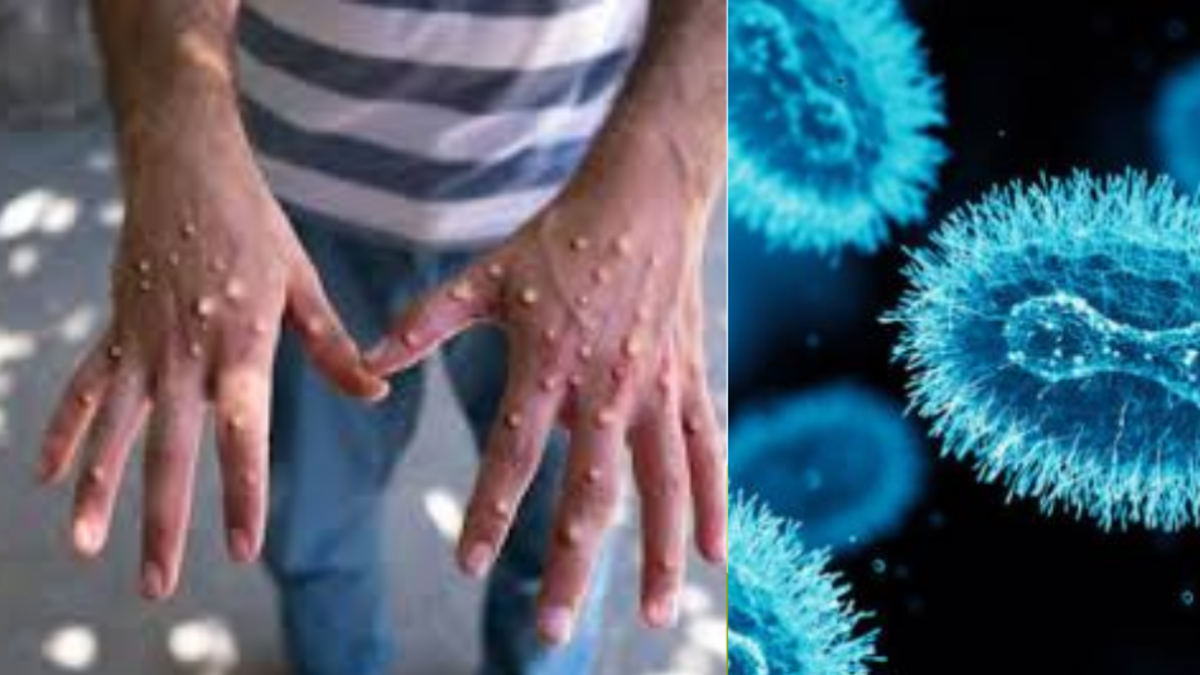
First Case of Mpox Clade 1B Confirmed in Colombia
Colombia’s Ministry of Health confirmed the nation’s first case of clade 1B mpox (formerly monkeypox) on April 18, 2026, detected in a traveler returning from Central Africa to Antioquia department. While public health officials urge calm, the emergence of this viral lineage—associated with sustained human-to-human transmission in endemic regions of Central Africa—necessitates heightened surveillance and rapid clinical assessment. The case underscores ongoing global concerns about viral evolution and spillover risk, particularly as clade 1B demonstrates distinct epidemiological patterns compared to the clade IIb variant that drove the 2022-2023 global outbreak.
Key Clinical Takeaways:
- Clade 1B mpox exhibits higher transmissibility and potential for severe disease compared to clade IIb, based on limited outbreak data from the Democratic Republic of the Congo.
- Current antiviral therapeutics (tecovirimat, brincidofovir) and vaccines (JYNNEOS, ACAM2000) retain expected efficacy against clade 1B, though real-world effectiveness data remain under active evaluation.
- Individuals with suspected mpox lesions or recent travel to endemic zones should seek immediate evaluation at specialized infectious disease clinics to enable prompt isolation, testing, and contact tracing.
The Nut Graf: Colombia’s detection of clade 1B mpox reveals a critical gap in genomic surveillance capacity within Latin American public health systems, highlighting the require for rapid diagnostic scaling and clinician education to prevent community transmission. Unlike the milder clade IIb strains that caused self-limiting rash illness in most healthy adults during the 2022 outbreak, clade 1B has been linked to higher rates of hemorrhagic manifestations, encephalitis, and fetal loss in pregnant individuals in Central African settings. This distinction demands a recalibration of clinical suspicion—particularly in patients presenting with atypical lesions, mucosal involvement, or systemic symptoms disproportionate to cutaneous findings.
According to genomic sequencing conducted at Colombia’s National Institute of Health (INS), the viral strain shares >95% homology with clade 1B viruses circulating in the ongoing Democratic Republic of the Congo outbreak, which has recorded over 14,000 suspected cases and 600 deaths since January 2023 per WHO situation reports. The virus enters host cells via membrane fusion mediated by the extracellular enveloped virus (EEV) form, utilizing glycosaminoglycans as attachment receptors before intracellular trafficking—a mechanism conserved across orthopoxviruses but potentially enhanced in clade 1B due to mutations in the A-type inclusion (ATI) protein gene, which may prolong environmental stability. These biological nuances inform why clade 1B warrants distinct public health messaging despite overlapping clinical presentations.
Funding for Colombia’s rapid response stems from the Pan American Health Organization’s (PAHO) Regional Emergency Fund, supplemented by a $2.1 million CDC cooperative agreement awarded in 2024 to strengthen zoonotic pathogen detection in Andean nations. This financial backing enabled same-day PCR confirmation at the INS reference laboratory using clade-specific probes developed during the 2022 outbreak. Crucially, no evidence suggests the patient transmitted the virus locally; all close contacts remain asymptomatic under monitored quarantine, reflecting effective initial containment.
“The identification of clade 1B in Colombia is not an unexpected development given global travel patterns, but it serves as a stress test for our diagnostic networks. Clinicians must recognize that while the rash may resemble varicella or syphilis, the presence of lymphadenopathy and centrifugal lesion distribution remains a key differentiator.”
Internationally, the WHO’s Strategic Advisory Group of Experts on Immunization (SAGE) maintains that pre-exposure prophylaxis with JYNNEOS vaccine is recommended for high-risk groups including healthcare workers treating orthopoxvirus patients and individuals with multiple sexual partners in outbreak zones—a guidance unchanged by clade 1B emergence. However, ongoing Phase II trials sponsored by Bavarian Nordic (NCT05471093) are evaluating intradermal dosing regimens to extend vaccine supply, with preliminary immunogenicity data showing non-inferior neutralizing antibody titers compared to subcutaneous administration. These studies, published in The Lancet Infectious Diseases in March 2026, directly inform Colombia’s current vaccine strategy for frontline responders.
For patients presenting with unexplained vesiculopustular rashes, particularly those with recent travel to Central or West Africa or known exposure to confirmed cases, immediate referral to specialized infectious disease units is critical. Facilities equipped for airborne isolation and PCR testing—such as those listed under board-certified infectious disease specialists—can initiate diagnostic workflows while minimizing exposure risk. Simultaneously, clinics managing sexual health services should update screening protocols to include mpox in differential diagnoses for genital or perianal ulcers, a nuance emphasized in recent CDC MMWR guidance.
The Body: Beyond individual case management, this event exposes systemic vulnerabilities in Latin America’s outbreak preparedness. Genomic surveillance remains uneven across the region, with only Brazil, Mexico, and Colombia maintaining routine sequencing capacity for orthopoxviruses—a limitation highlighted in a 2025 PLOS Medicine analysis of pandemic readiness indicators. Strengthening laboratory networks through PAHO’s Integrated Disease Surveillance and Response (IDSR) framework requires sustained investment, yet offers substantial returns by enabling early detection of not just mpox, but also emerging threats like Oropouche virus or Mayaro virus.
From a therapeutic standpoint, tecovirimat remains the first-line antiviral for severe or high-risk mpox cases, though access barriers persist in low-resource settings. The NIH-funded STOMP trial (NCT04556537), which concluded in 2024, demonstrated that while tecovirimat reduced lesion duration by a median of 2.1 days in clade IIb infections, its efficacy in immunocompromised subgroups was inconclusive—a finding driving current research into combination regimens. Clinicians treating suspected clade 1B cases should consult local pharmacovigilance channels for updated dosing guidelines, particularly when considering brincidofovir in patients with hepatic impairment.
Public communication must balance transparency with avoidance of stigma. Historical parallels to early HIV/AIDS messaging reveal how premature associations between disease and specific populations can undermine trust and delay care-seeking. Colombia’s health ministry has appropriately framed this case within a travel-associated context, avoiding language that could stigmatize affected communities—a practice aligned with WHO risk communication best practices. Nevertheless, clinicians should proactively offer testing to anyone with compatible symptoms regardless of perceived risk, as asymptomatic or paucisymptomatic transmission, while less documented for clade 1B, cannot be ruled out.
The Editorial Kicker: As global travel resumes pre-pandemic volumes, the detection of clade 1B mpox in Colombia reinforces that pathogen surveillance cannot be confined to traditional endemic zones. Strengthening diagnostic readiness, maintaining vaccine stockpiles, and fostering clinician vigilance constitute a durable defense against not only orthopoxviruses but also future zoonotic threats. For healthcare facilities seeking to update their outbreak response protocols or individuals needing post-exposure evaluation, connecting with vetted local public health clinics ensures access to evidence-based guidance and timely interventions.
*Disclaimer: The information provided in this article is for educational and scientific communication purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider regarding any medical condition, diagnosis, or treatment plan.*
