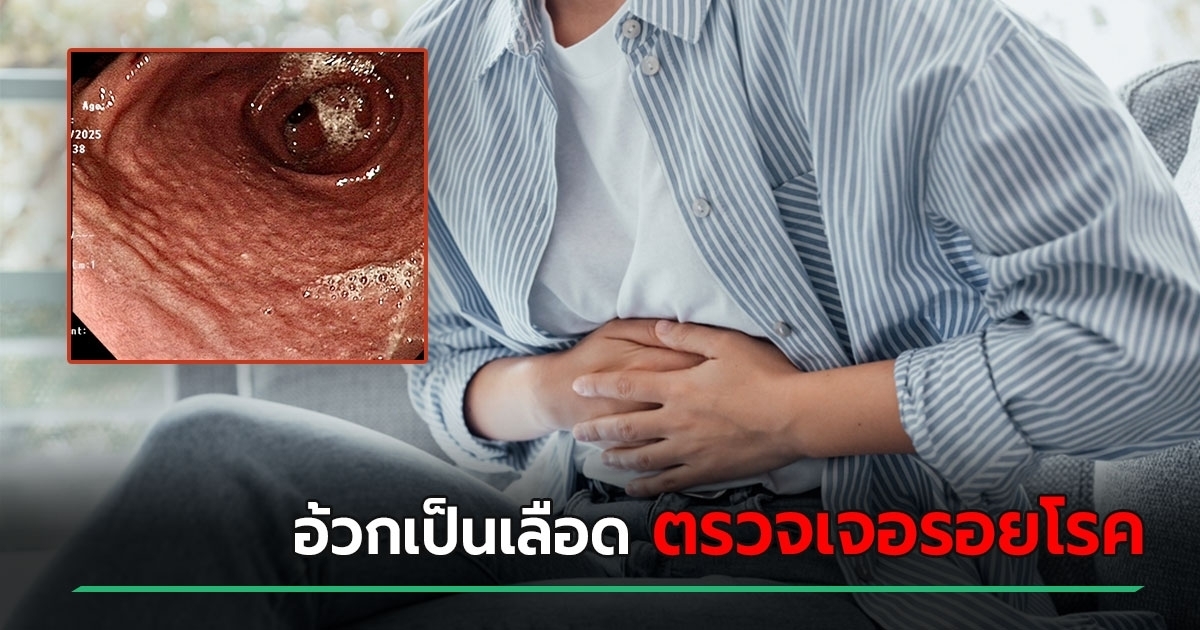
Child Vomits Blood: Doctor Finds Small Nodules in Stomach Signaling Serious Illness
A sudden episode of severe hematemesis in a 15-year-old boy has surfaced as a critical clinical warning, revealing the presence of small, pebble-like nodules within the stomach. While initial suspicions often lean toward the accidental ingestion of foreign objects, medical evaluation confirmed these growths were internal, signaling a potentially malignant progression toward gastric cancer.
Key Clinical Takeaways:
- Severe vomiting of blood (hematemesis) in adolescents is a medical emergency requiring immediate diagnostic intervention.
- The discovery of internal, nodular growths resembling “pebbles” during endoscopy can be a primary indicator of serious gastric pathology or malignancy.
- Early detection through endoscopic visualization is the standard of care to prevent the progression of gastric lesions into advanced-stage cancer.
The clinical presentation of this case—a teenager admitted with sudden, violent vomiting of blood—highlights a dangerous intersection of pediatric health and oncology. Upon performing a gastroscopy, clinicians identified small protrusions on the stomach lining. The distinction made by the medical team was pivotal: these were not ingested stones, but rather biological growths. This distinction shifts the diagnosis from a simple foreign body obstruction to a complex oncological risk, where the “pebbles” serve as early markers for gastric cancer.
The Pathogenesis of Hematemesis and Systemic Warning Signs
Hematemesis, the act of vomiting blood, is rarely an isolated symptom and typically indicates a significant breach in the gastrointestinal mucosa. In the case of the 15-year-old patient, the severity of the bleeding suggests a rapid erosion of the stomach lining. When the gastric wall is compromised by nodules or malignant growths, the resulting hemorrhage can lead to systemic instability. Clinical observation of such patients often reveals a constellation of symptoms that signal hemodynamic compromise.
The presence of hematemesis, combined with dizziness, nausea, and abdominal pain, necessitates urgent triage. When blood is lost rapidly, patients may exhibit pale skin, cold extremities, and an increased heart rate as the body attempts to compensate for reduced blood volume.
Beyond the visible blood, medical professionals monitor for “coffee-ground” emesis—blood that has been partially digested by gastric acid—and melena, which manifests as black, tarry stools. These markers, alongside decreased urine output and rapid, shallow breathing, indicate that the patient may be entering a state of shock. For families noticing these signs in children, the priority is immediate stabilization through specialized pediatric clinics to prevent fatal outcomes.
Differential Diagnosis: Distinguishing Benign Lesions from Malignancy
The discovery of “pebbles” in the stomach requires a rigorous differential diagnosis to separate benign conditions from life-threatening diseases. While the news highlighted the risk of gastric cancer, several other pathologies can cause similar mucosal disruptions. Severe gastroesophageal reflux disease (GERD), deep gastric ulcers, or esophageal tears (Mallory-Weiss tears) can all trigger significant bleeding. In some cases, esophageal varices—dilated veins that can rupture—present a similar emergency profile.
However, the specific morphology of the “pebbles” described in this case suggests a proliferative process. Unlike an ulcer, which is an erosive pit, these nodules represent an abnormal growth of tissue. This is where the role of the board-certified gastroenterologist becomes indispensable. Through high-definition endoscopy, clinicians can differentiate between inflammatory polyps and malignant neoplasms. The ability to visualize these nodules in real-time allows for immediate biopsy and, in some instances, the use of cauterization to stop active bleeding.
The Critical Role of Endoscopic Intervention and Early Screening
The standard of care for suspected gastric malignancy involves a multi-step diagnostic pathway. Endoscopy is the gold standard, providing not only a visual map of the stomach lining but as well the means to extract tissue samples for histopathological analysis. For the 15-year-old patient, this procedure was the only way to uncover the “hidden” cause of the hemorrhage. Without this intervention, the nodules might have remained asymptomatic until the cancer reached an advanced stage, significantly increasing morbidity.
The public health implication of this case is a call for increased vigilance among parents and guardians. Gastric cancer is often perceived as a disease of older adults, but the emergence of pediatric and adolescent cases underscores the need for early screening when red-flag symptoms appear. The biological mechanism of these nodules often involves chronic inflammation or genetic predispositions that accelerate cellular mutation. To ensure an accurate diagnosis, patients are often referred to advanced diagnostic imaging centers for complementary CT scans or endoscopic ultrasounds to determine the depth of the lesion’s penetration into the gastric wall.
Clinical Trajectory and Future Preventative Outlook
The trajectory of gastric pathology in young patients is often aggressive, making the window for successful intervention narrow. The transition from small mucosal nodules to invasive carcinoma can occur rapidly if the underlying cause—whether infectious or genetic—is not addressed. Current clinical consensus emphasizes that any instance of unexplained hematemesis must be treated as a high-risk event until proven otherwise.
Looking forward, the integration of more sensitive biomarkers and non-invasive screening tools may allow for the detection of these “pebbles” before they trigger a hemorrhagic event. The goal of modern gastroenterology is to shift the diagnosis from the emergency room to the screening clinic. By identifying pre-cancerous nodules in their earliest stages, the medical community can employ minimally invasive resections, drastically improving the survival rate and quality of life for young patients.
For those managing chronic gastric symptoms or seeking a second opinion on diagnostic findings, consulting with a multidisciplinary team of oncologists and surgeons is the most prudent path forward. Ensuring that care is coordinated through vetted medical professionals is essential for navigating the complexities of a potential malignancy diagnosis.
*Disclaimer: The information provided in this article is for educational and scientific communication purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider regarding any medical condition, diagnosis, or treatment plan.*
